Welcome to “My Corneal Save,” a magazine department that provides a firsthand account of a memorable cornea case and how the ophthalmologist was able to help the patient.
A 66-year-old Caucasian woman presented with blurry vision and intolerable photophobia and glare OU. She said she observed diurnal fluctuation in her vision throughout the day, and that she was contact lens intolerant. Additionally, the patient said she had a prior distant history of radial keratotomy (RK) with resultant typical progressive hyperopic shift and progressive irregular astigmatism. She further divulged she’d had an interval LASIK enhancement OU.
Exam Findings
Best spectacle-corrected visual acuity (BSCVA) was 20/50 OD and 20/40 OS. Exam disclosed an 8-cut RK OU with irregular, scarred incisions OU (see Figure 1). Moderately dense nuclear cataracts were seen OU.
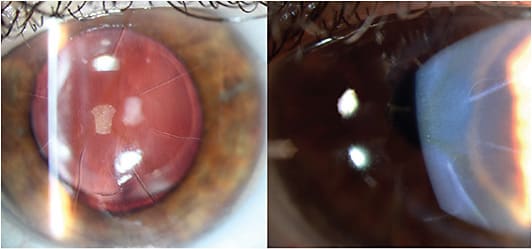
Topography showed an 11 D range across the central 3 mm of her corneas. Irregular astigmatism was obvious, OU, OS > OD, nearing the visual axis.
OCT testing of the macula OD showed a thick epiretinal membrane that had foveal distortion and macular thickening.
Diagnosis
Based on exam findings, the patient was diagnosed with increasing cataracts OU and irregular astigmatism in both eyes.
Management
The patient elected to undergo cataract surgery OU, combined with a pars plana vitrectomy and membrane peeling OD. A monofocal IOL with negative asphericity was used. Postoperatively, her VA was modestly improved OU, with BSCVAs of 20/60+2 OD and 20/40 OS.
Despite these surgical interventions, the patient reported that she was still horribly photophobic, had profound glare, and had notable diurnal fluctuation in her vision.
Given her contact lens intolerance and her limited, unsuccessful conservative options, an FDA compassionate use device exemption for a “piggyback” pinhole implant was sought and granted.
This back acrylic implant (XtraFocus implant, from Morcher), designed for either sulcus or in-the-bag placement, sits anterior to a separate IOL. The implant is opaque to white light, but transparent to infrared light, thus, permitting unimpeded imaging with infrared testing equipment, such as ICG fundus cameras and OCT machines. Slit lamp biomicroscopes fitted with infrared light sources and cameras permit visualization through the implant material.
The “piggyback” pinhole implant was placed uneventfully OD, resulting in a 20/20-1 uncorrected result. (see Figure 2) After implantation, the patient noted dimness and a prominent, discrete circular halo. Regardless, she said she felt the implant had significantly improved her vision.
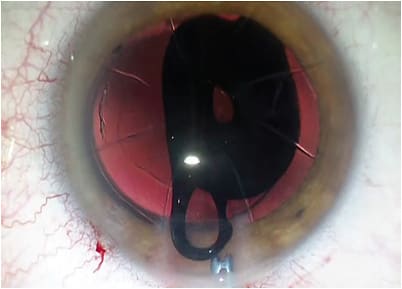
Over the next 9 months, the patient said she gradually adapted to the implant, though still reported dimness at night and the halo. Again, despite this, she stated that the improvement in her quality of vision was such that she requested the same device be placed OS.
Regarding the halo, diffraction from pinhole edges has been revealed as a cause. Additionally, some implanted patients also report dimness of vision due to the diminished amount of total light entering the eye, though this phenomenon is mitigated by both the directional sensitivity of the cones, as described by the Stiles-Crawford effect, and relative upregulation of photoreceptor pigments.
A “piggyback” pinhole implant was placed OS uneventfully, and the patient regained 20/30 uncorrected and 20/20 best-corrected vision with a +0.50 +0.25 x 060 lens.
Her uncorrected near vision was J5 OD and J3 OS. After some time, the patient said she felt her “brain had adapted” to the implants and that, “sometimes” she doesn’t notice halos at all. A 5-line improvement in (uncorrected and) best-corrected VA with the pinhole implant is especially impressive, given that her maximally constricted pupil was already reasonably small. The pinhole accounts for 56% of this aperture by area (see Figure 3).
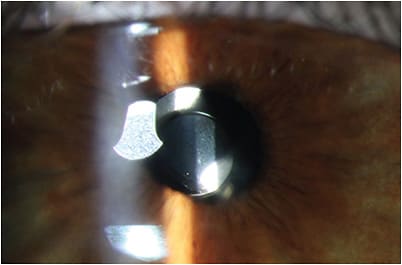
In addition to the XtraFocus implant, a spherical, monofocal IOL containing an embedded pinhole aperture (Apthera IC-8, from Bausch + Lomb) is available. This is designed for improved depth of focus in presbyopic patients, though it may also prove useful in aberrated corneas. Its one-piece, hydrophobic, sharp-edged acrylic design requires placement at the time of cataract surgery.
Certainly, rigid gas permeable contact lenses or other rigid hybrid or scleral contact lenses can be helpful in patients who are able to tolerate contact lens wear, unlike the patient described.
Further, some surgeons advocate for deep anterior lamellar keratoplasty or penetrating keratoplasty for aberrated corneas. Corneal transplantations are an option, yet they have their own non-trivial risks and limitations, sometimes, perhaps, with similar aberrations from some underlying pathologies.
Similarly, keratoprostheses have their own challenges, though new “softer” iterations may be better tolerated by patients.
Outcome
In this patient, the optical benefits of the pinhole implant outweighed the downsides of diffractive halos. Accordingly, clinicians should keep these features in mind when considering utilizing pinhole optics and their alternatives. CP

DR. SNYDER is a member of the Board of Clinical Governance, Cincinnati Eye Institute, chair of clinical research steering committee, and professor of ophthalmology at University of Cincinnati, in Cincinnati, Ohio.








